To our valued patients, with regards to the situation in Alabama Read More
- Chattanooga: 423.899.0500
- Knoxville: 865.692.3433
- Chattanooga: 423.899.0500
- Knoxville: 865.692.3433
To our valued patients, with regards to the situation in Alabama Read More
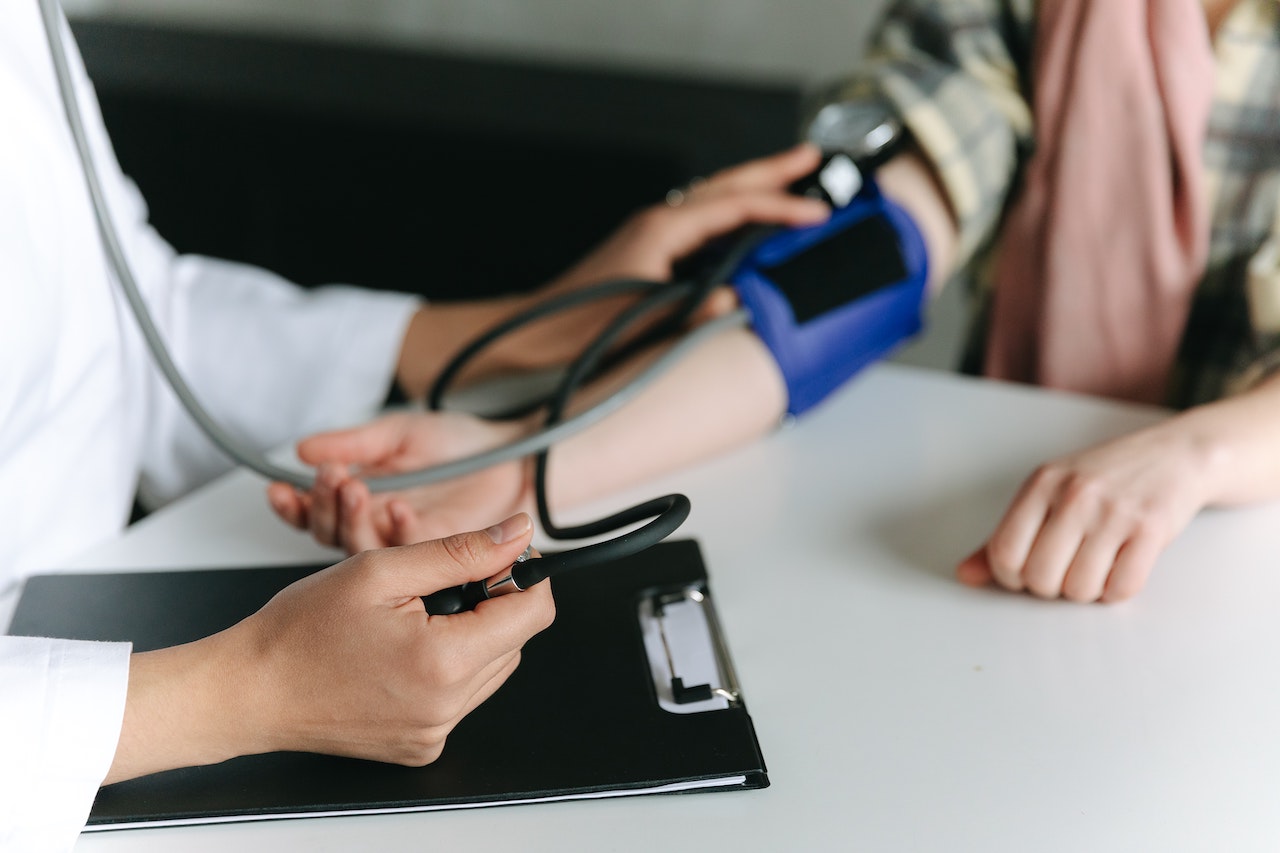
One of the most common diagnostic fertility tests, the hysterosalpingogram, more commonly referred to as the HSG, is used to evaluate the condition of the fallopian tubes. While it is a standard component of most fertility evaluations, it’s also one of the tests that patients have the most questions about. To help clear things up, Dr. Donesky is sharing some information about the different types of HSG tests and how they help doctors diagnose issues that may affect a woman’s fertility.
(Image from https://parenting.firstcry.com/articles/natural-treatment-for-blocked-fallopian-tubes/)
Traditionally, the way we tested to see if the fallopian tubes were open was with the injection of x-ray contrast fluid into the uterus and fallopian tubes. We would see a nice outline of the uterine cavity as well as the tubes and could tell if the fluid passed all the way through the tubes into the pelvis. If the contrast fluid was evenly distributed in the pelvis, we could also imply that there were no significant adhesions, or scar tissue, around the tubes.
While this was a good test, it had some disadvantages. First of all, the actual uterus and tubes do not show up on x-ray – only the contrast fluid shows up, so you would not see fibroids or ovarian cysts. It also involved exposure to a small dose of radiation and was inconvenient, as it had to be scheduled in a radiology suite.
The ultrasound version (sono-HSG or sonohysterogram) is sometimes often referred to simply as the FemVue, the brand name of a device used to perform the procedure. Today, it’s the most commonly used test for evaluating the fallopian tubes. This version of the procedure is performed in the office and in an exam room with equipment designed specifically around the gynecologic exam, which can make it more comfortable for the patient. It does not involve x-ray or contrast fluid (which can rarely cause allergic reactions) but instead uses only sterile water or saline and air bubbles. With 3-D ultrasound equipment, we can get an excellent view of the uterus itself as well as the interior cavity and manipulate the image on the screen to get a more complete picture. It will also show the ovaries and any cysts on them.
While the tubes are difficult to see with ultrasound alone, the addition of air bubbles to the water allows us to track the bubbles through the tubes and document that they are open. It is less effective in testing for adhesions around the tubes than the x-ray test, but for the initial screening of the pelvis, it is an excellent test.
The HSG test is mostly used to see if the fallopian tubes are open. It can also be used to check if there congenital uterine anomalies, fibroid tumors, polyps, or uterine scar tissue. during the test, the doctor normally checks the fallopian tubes if they have defects in them along with if there is pelvic scar tissue in the abdominal cavity near the tube.
Endometriosis is not well seen on either the x-ray or the ultrasound version of the HSG, but if there are cysts of endometriosis tissue in the ovaries (called endometriomas), the ultrasound procedure will generally be able to detect those. As mentioned previously, if there is scar tissue from prior surgeries or possibly from severe endometriosis, the x-ray test may be better at detecting that. Of course, the best test for endometriosis is a laparoscopy, which involves surgery and is best reserved for patients whose symptoms are highly indicative of endometriosis, or who have a history of prior pelvic surgeries.
There is absolutely no preparation needed for the HSG test. It can be helpful to take some ibuprofen about 30-60 minutes ahead of your appointment time to reduce cramping. If you have someone that can drive you home after the test, a muscle relaxant like Valium may help to relax the openings of the tubes and make it less painful to push fluid into them.
The ideal time to have an HSG is right after your period is over (when the uterine lining has been shed and is as thin as it will ever be). This makes it easier to see the uterus and tubes on the ultrasound. You should call the office to schedule the test between days 6 and 11 of your cycle.
Most insurance policies will cover the HSG. However, if you do not have insurance and the procedure is performed in-house, the cost at The Fertility Center for the HSG test is $525. This is less than the cost of an outpatient procedure, which will include charges for the facility and the procedure itself. We offer the HSG test for clients nationwide, but most of our customers come from Nashville, Knoxville, Atlanta, and Chattanooga.
Both versions of the HSG put enough fluid into the uterus to separate the walls and stretch the cavity. This can cause cramps and will produce some pain. As long as the fluid is introduced slowly so that the cavity is not forced open, the pain will be minimal. Most women will actually state that they expected it to be much worse. The procedure itself will feel like a bad period cramp for about 30-45 seconds. Once the catheter is removed, the pain will end for most women almost immediately.
Some women will continue to have milder cramping for 15-20 minutes following the procedure. There may also be a small amount of fluid expelled immediately following the test, but the amount of fluid injected is usually only about two to three teaspoons, so this is minimal. It is important to keep in mind that severe cramping after the procedure (especially later in the day) or fevers afterward are abnormal. If either of these occur, contact the doctor’s office immediately.